Kinesiology is the study of human movement, performance, and function. In Canada, kinesiology is a professional designation as well as an area of study. Kinesiology applies the sciences of anatomy, physiology, biomechanics and neuroscience to understand and improve movement, performance and function through active rehabilitation (exercise).
Individual Kinesiology sessions are delivered by a Kinesiologist who is certified by the B.C. Association of Kinesiologists, with focus on general activation, mobility, strength and conditioning. Both gym-based and pool-based (hydrotherapy) sessions are offered.
Prior to seeing a Kinesiologist, clients are seen by one of our Physiotherapists to ensure that kinesiology is an appropriate intervention for them. The Kinesiologist will then developed and monitor a personalised, progressive exercise program.
Good bike fit is essential for ensuring comfortable, injury free cycling, as well as for maximising power and efficiency. Knee pain, back pain and neck/shoulder pain are all common in cyclists. These may be the result of an old injury or biomechanical issues, or may be related to bike position. Many of these issues can be addressed by combining an orthopaedic physical examination with a dynamic evaluation of cycling position. Phil Burman, physiotherapist at Dale Charles Physiotherapy has experience setting-up over 1000 cyclists from recreational to national level, as well as over 20 years of experience as a road cyclist and mountain biker.
The ‘Physiotherapy Bike Fit’ service is conducted as an extended consult in the clinic. If the goal is injury prevention and rehab, your extended benefits plan may cover all or part of the cost

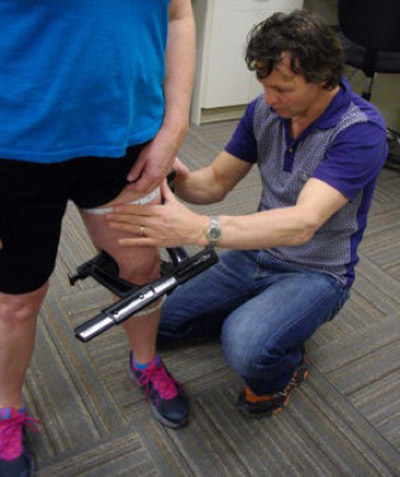
DonJoy is the leading brace manufacturer in North America. Our physiotherapists are trained in the measurement and fitting of custom-made and off the shelf braces for a variety of orthopedic and sports injuries. After injury or surgery, joint and soft tissue support may be indicated for a safe return to sport, work or daily activity.
Available bracing products include the following:
• DonJoy Knee Braces: functional knee braces are designed to assist unstable knee conditions such as ACL injuries and reconstructions. Custom and off the shelf braces are available. • OA Unloader Knee Braces: designed to unload arthritic knee joints to assist in daily activity. Custom and off the shelf braces are available. • Ankle braces • SI joint supports • Elbow straps • Wrist supports • Shoulder stabilization • ‘Core Shorts’ for hip strains • Orthopedic walking boots
A Certified Hand Therapist is on staff to create custom splints for post-operative recovery of hand and upper limb conditions. This is a unique service provided by a highly trained and experienced physiotherapist with advanced training and credentials in hand therapy.
Concussion is a form of mild traumatic brain injury, and concussion in sport has created significant social awareness of the need for prevention, recognition and management of head injuries. Motor vehicle accidents, work injuries and falls can also cause concussion.
Our clinic has been instrumental in creating Concussion Protocols for local sport organizations, such as soccer and Jr A hockey. In addition, we created a Concussion Protocol for the 2016 BC Winter Games held in Penticton. It is recommended that all sport organizations have a Concussion Protocol in place to guide coaches, parents and players on recovery plans that keep up with current information.
Recovery from concussion requires a knowledgeable healthcare team. Our clinic staff have completed recognized courses on concussion management, and are able to guide clients of all ages through recovery protocols.
For the few clients that have persistent concussion symptoms beyond the expected recovery timelines, we can provide assessment and treatment aimed at assisting in the recovery. As part of the healthcare team, physiotherapists provide treatment for balance, visual disturbance, graded exercise, and return to sport or work. In addition, manual therapy may have a role in treatment of persistent headache related to neck trauma at the time of injury.
ACUPUNCTURE has its roots over 4000 years ago to treat a host of ailments under the philosophies of oriental medicine. This type of acupuncture falls under the category of Traditional Chinese Medicine (TCM), and generally provided by registered acupuncturists.
However, since the 1970’s, acupuncture has become more familiar and common place in North America for treatment of many types of musculoskeletal injuries, including sports injuries, whiplash, post-surgical pain, osteoarthritis and other types of physical trauma. This Western culture approach to treatment with acupuncture is commonly referred to as Anatomical or Medical acupuncture.
The Acupuncture Foundation of Canada Institute (AFCI ) is a well-known and respected educational organization that trains most of the physiotherapists in Canada (as well as many medical doctors, nurses, dentists and chiropractors) who use an anatomical approach to acupuncture. Other programs are recognized at University of Alberta and McMaster University.
In very simple terms, this anatomical approach uses the traditional acupuncture points on the body to help decrease inflammation, pain, muscle spasm and tightness in order to increase mobility and reduce recovery time from an injury or other physical problems.
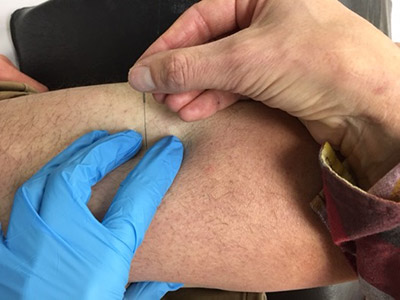
DRY NEEDLING has emerged as a popular physiotherapy treatment for myofascial pain but differs from acupuncture in that needle insertion points are not limited to acupuncture theory. Vancouver physician, Dr. Chan Gunn made a significant contribution to the study and treatment of pain related to neuropathic changes and muscle sensitivity. His IMS (intramuscular stimulation) technique using a single acupuncture needle to treat multiple pain areas remains the foundation of many of the other dry needling education programs that train physiotherapists. FDN (Kineticore functional dry needling) and GTT (Gokavi technique) are examples of other dry needling approaches.
Physiotherapists in the group have training in dry needling (IMS, FDN, GTT), some with both acupuncture and dry needling certification. Combined with manual therapy, pain education and exercise, clients are receiving leading edge treatment from experienced and qualified therapists.
Certified Hand Therapists (CHTs) are physical therapists or occupational therapists who specialize in the physical rehabilitation of hands, wrists, elbows and shoulders affected by injury, surgery, or naturally occurring conditions such as arthritis. CHTs also have the unique skill of the fabrication and provision of custom upper extremity splinting - these are made right in our hand therapy clinic and individually crafted to fit each patient.
Custom splints often help patients with different types of pathology including:
• Tendinopathy (i.e. tennis elbow, de Quervain and trigger finger) • Neuritis (i.e. carpal tunnel syndrome) • Joint pain (i.e. thumb arthritis) • Muscle strain and ligament sprain (i.e. skier’s thumb) • Post-surgical protocols (i.e. flexor tendon repairs) • Healing fractures in the hand, wrist and arm.
We have a passion for treating the upper extremity. We know people value the use of their hands and any loss of function through injury or accident may have a devastating effect on their lives. Anyone with an injury wants the best treatment for optimal recovery. The Certified Hand Therapist credential is recognized by many professional organizations as a benchmark for excellence, and offers assurance to the public that we have achieved a high level of competency in the profession.
Neurological rehabilitation is an important part of recovery following a Central Nervous System (CNS) disorder. For patients living with functional limitations related to nervous system damage, physiotherapists work to restore safe and independent function. Treatment is frequently focused on improving mobility and functional activities such as sitting, standing, balance, walking, and upper limb function, as well as higher level activities, following a stroke (CVA), spinal cord injury (SCI) or acquired brain injury (ABI). In the case of progressive pathologies, the goal is to maintain function and independence.
An understanding of the altered neurology following CNS disorder, combined with a detailed knowledge of the musculoskeletal system, allows physiotherapists to effectively use therapeutic exercise, physical modalities and other personally tailored interventions in a safe environment.
Neurological rehabilitation is demanding in terms of time, support and funding. With the help of a multi-disciplinary team, it is common to see significant improvement in function, safety and independence.
Manual Therapy is the ‘art of the science’ of physiotherapy. It defines the hands-on techniques that therapists use to assist in the recovery of movement through joint mobility and muscle re-education.
Our therapists have spent many post-graduate hours studying the practice of manual therapy techniques, including mobilization and manipulation of limbs and spinal segments. Physiotherapy courses lead to advanced training and certification levels. We as a group provide expert treatment by combining orthopaedic manual therapy with exercise, pain management and education.
Rehabilitation from injury, illness or surgery may also require additional physical modalities such as dry needling and acupuncture, ultrasound, laser, electrical current for neuromuscular activity, heat and ice. These additional modalities may be used as adjuncts to manual therapy treatment.
Therapeutic exercises are frequently prescribed for further strength and mobility. Together with the client, a treatment plan is developed to assist in reaching a goal of maximum recovery.
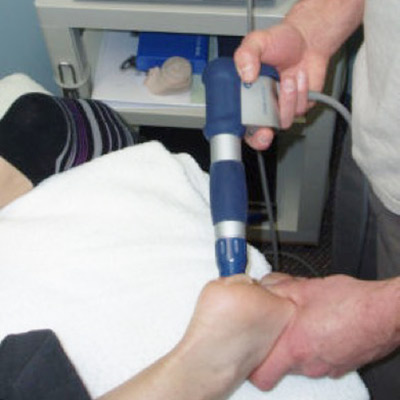
Shock wave therapy (SWT) is technology derived from ‘lithotripsy’; a technique to break down kidney stones using sound wave energy. In the 1990’s, SWT was found to be successful in treating certain musculoskeletal conditions. Radial shock wave therapy (rSWT) delivers a low-energy shock wave. It has evolved from more expensive medical technology.
The energy of rSWT is produced by a low frequency ballistic compression, creating an acoustic sound (or pulsed pressure) ‘shock wave’. The shock wave is directed at the selected treatment site to stimulate metabolism and enhance circulation. The shock energy assists disorganized tissue to gradually recover through tissue regeneration and repair models. Treatment sessions are short and moderately uncomfortable. rSWT is safe, and can be used by a physiotherapist in the treatment of musculoskeletal disorders.
Conditions that benefit from SWT: Research is accumulating in the use of pulsed pressure rSWT. Evidence supporting its use has been published in high quality medical journals. The strongest evidence is for shoulder calcific tendinitis and plantar fasciitis, but satisfactory results have been published for other common musculotendinous problems that have ‘failed to respond’ to other conservative treatment. rSWT is a non-surgical option with results that match surgical outcomes, and should be considered when other treatment options have failed.
• 87% Shoulder tendinopathy (with or without calcification) • 86% Plantar fasciitis • 86% Achilles tendinopathy (including insertional) • 69% Tennis/Golfer’s elbow • 58% Patellar tendinopathy
Currently, the Dale Charles Physiotherapy group is the only physiotherapy provider using rSWT in the Okanagan.
Injury prevention and enhancing performance are fundamental parts of treatment before a sports injury sidelines an athlete. Our team of physiotherapists is able to identify weaknesses and movement faults that if left unchecked, can lead to reductions in performance and injuries. Staff have taken courses on Functional Movement Screening and Selected Functional Movement Assessment to assist in assessing movement, strength and performance.
Our therapy group have provided knee injury prevention programs for athletes from a wide range of sports, incorporating a neuromuscular training program that has been demonstrated to reduce serious knee injuries by up to 80%.
We have also been involved with concussion awareness programs, and have provided concussion protocols for groups such as local soccer, Jr hockey and BC Winter Games. Therapists in the group are involved with ongoing continuing education on concussion management and keep abreast with current research in the area of concussion.
We continue to provide experienced consulting to the Penticton Vees Jr Hockey team, and side-line coverage for events such as rugby and soccer in the community. Some of our staff maintain certification in Sports Physiotherapy, and travel with National teams, such as rugby, snowboard and alpine skiing.
The Sports Clinic was the site of the Athlete’s Clinic for the 2016 BC Winter Games in Penticton, with staff taking lead roles on the organizing committee for Medical Services in positions of Medical Director, Physiotherapy Chair and Chair of Medical Volunteers, as well as attending to athletes on the sidelines at events.

50% of adults will experience symptoms of dizziness their lifetime. Dizziness and balance problems represent 10% of all physician visits, and is the #1 reason for physician visits for patients >65 years.
Vestibular Rehabilitation is the assessment and treatment of vestibular disorders following a diagnosis of complaints of dizziness and ‘true’ vertigo. BPPV (benign positional paroxysmal vertigo) is the most common cause of vertigo, accounting for up to 30% of vertigo patients.
Therapists on staff are trained to screen patients with complaints of dizziness or vertigo in order to determine which clients will respond to therapy (such as habituation exercise or canal repositioning manoeuvres); or will require further medical investigation.
Extended visits are required to fully assess and treat a client with vestibular disorders.